You're in good hands
With an in-depth knowledge of the body and how it works along with specialized hands-on clinical skills to assess, diagnose and treat symptoms of illness, injury or disability.
With an in-depth knowledge of the body and how it works along with specialized hands-on clinical skills to assess, diagnose and treat symptoms of illness, injury or disability.







I have completed extensive training in manual therapy, successfully completing a post-graduate fellowship in Orthopaedic Physiotherapy through the Canadian Academy of Manipulative Physiotherapist (CAMPT).
CAMPT is one of the leaders in post-graduate manual therapy coursework in Canada. Manual therapy is a specific approach to physiotherapy that focuses on hands-on joint mobilizations and manipulations aimed at decreasing pain, increasing joint mobility, and restoring proper muscle activation.
What separates the CAMPT program from other professional development courses is its hierarchical progression of coursework as well as its internationally-recognized qualifications and regulations through a rigorous examination process.
By being an active member of the Canadian Academy of Manipulative Physiotherapist, this ensures my continued advancement in orthopaedic physiotherapy through clinical mentorship and training which meets and exceeds the international standards in Physiotherapy.
Concussion management is an ever-evolving discipline that requires a comprehensive, individualized, and evidence-informed approach. Given the complex and often overlapping nature of post-concussion symptoms, effective care relies on a multidisciplinary framework that addresses not only the injury itself, but the various systems that may be contributing to symptom persistence.
As a physiotherapist with advanced training, including a CAMPT manual therapy designation and specialized vestibular rehabilitation expertise, I am able to perform a focused and efficient assessment of key systems commonly affected following concussion. This includes evaluation of the vestibular system (balance and spatial orientation), oculomotor function (eye tracking and coordination), and the craniovertebral region of the cervical spine, all of which can play a significant role in ongoing symptoms such as dizziness, headaches, visual disturbances, and neck pain.
Treatment is guided by clinical findings and typically involves a combination of targeted therapeutic exercise, manual therapy, and patient education. Emphasis is placed on symptom-guided progression, pacing strategies, and empowering patients with the tools needed to manage flare-ups and gradually return to daily activities, work, and sport.
Recognizing that concussion recovery is rarely linear and often multifactorial, ongoing communication with your primary care provider is maintained to ensure coordinated care. When appropriate, timely referrals are made to other healthcare professionals with specialized expertise. These may include a Registered Vestibular Therapist, Neuro-ophthalmologist, Occupational Therapist, Kinesiologist, ENT specialist, Neuropsychologist, or Counsellor. In some cases, further medical evaluation by your general practitioner may be recommended to rule out or investigate contributing factors.
Ultimately, successful concussion management reflects a collaborative effort—one that integrates multiple perspectives and skill sets to ensure all aspects of the patient’s recovery are addressed.
Temporal Mandibular Disorder (TMD), or as it is often referred to as simply TMJ (Temporal Mandibular Joint) refers to jaw and fascial pain located at or near the TMJ. Your TMJ is the joint where your jaw meets the side of your head and is one of the most complicated joints in the body. This dysfunction can cause a number of issues related to teeth health and jaw movements. If this joint doesn’t function properly, you may experience painful chewing, pain with yawning, jaw stiffness, locking or popping feeling in your ear with opening or closing, or simply just pain near your joint. If left untreated, TMD can lead to chronic, long term pain as well as symptoms of migraines or tinnitus, which is a slight ringing in your ear.
I have done post-masters training specializing in up-to-date revolutionary therapy techniques and proven treatments that provides my patients with the knowledge and care to reduce their TMJ pain and improve the functional movement of their jaw.
The evaluation will take roughly an hour and a half over 2 visits; 60mins on day-1 and 30mins on day 2. This allows you to split the cost to your health insurer if applicable. The majority of our first consult is to determine the full onset of symptoms as well as getting an in-depth medical history, including a clear dental history. The next most important aspect of treatment is education, as the jaw can only begin to heal once it is properly unloaded. Lastly, I will assess the movement of the jaw and test the muscle balance of the jaw’s stabilizing forces. Due to importance that your medical history and education plays in the success of your treatment, our initial consult can be in clinic if you so choose, however for immediate treatment, it is recommended to book your initial assessment via tele-health to get you on the road to recovery sooner.
After this initial consultation, you will receive a treatment plan specific to your needs and a follow up will be booked. Treatment will include corrective exercises as it pertains to the proper opening and closing of the jaw as well as using hands-on mobility techniques, which when combined promotes the essential principles of motor learning. This combined approach will teach you how to optimize your movement to make opening and closing more easily and rapidly accomplished.

Golf presents unique challenges to the body. It is a sport that combines a high-intensity and high-skill activity with a history largely void of understanding the benefits and importance of “Golf Fitness”.
Golf Fitness isn’t about looking like the best player on Tour. It’s about being fit to play the game at an individual’s highest ability and doing so without causing injury. It’s about understanding how a body’s limitations can influence the golf swing and how to address those limitations through the proper channels; whether it’s through swing instruction or physical- medical screening, or both. It’s about understanding the latest technology and how that technology can be implemented to increase performance. How do you get this knowledge to help players get fit to play their best golf? Through TPI Certification.
TPI has spent almost two decades studying one thing – the Body-Swing Connection™. TPI professionals have one simple philosophy. We don’t believe there is one way to swing a club, rather there are an infinite number of ways to swing a club. But we do believe that there is one efficient way for everyone to swing a club and it is based on what they can physically do; which is controlled by one’s own body’s abilities and limitations.
Is pain limiting your swing or your ability to navigate the course? As a TPI Medical Professional, I use golf-specific injury assessment tools and rehabilitation techniques to get players back in the game quickly. Not injured? Not a problem! There are certain swing characteristics associated with the golf swing that are precursors to pain and injury. Few understand how to identify these characteristics better than a TPI Medical Professional. So whether it’s determining how these injuries developed, developing specific rehabilitation techniques to treat these injuries or determining how specific physical limitations can be addressed to improve performance and prevent future injuries, a TPI Medical Screen will keep you in the game longer!
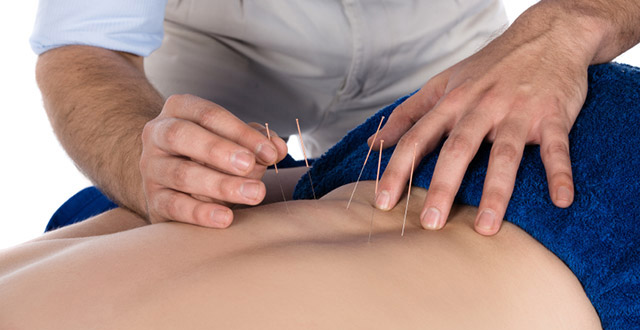
Intramuscular Stimulation (IMS), also known as Functional Dry Needling or simply Dry Needling, consists of inserting a very thin mono-filament needle into a Myofascial Trigger Point. It is a therapeutic treatment used primarily to reduce local and widespread pain by deactivating hyper-sensitized nerves, increasing blood flow, and stimulating the body’s own healing capabilities. IMS can further be used to improve function and proper movement patterns by increasing range of motion and restoring healthy muscle activation.
Some common conditions that I treat with IMS are Neck and Back pain, headaches either caused by migraines or cervicogenic in nature, Post-Concussion Syndrome, as well as any number of other muscular-skeletal conditions of the body.

The Functional Movement Screen (FMS) is an objective screening tool that measures seven fundamental movements that are key to life. The FMS aims to identify asymmetries of functional patterns that measures a whole body’s mobility, stability and how they interact together during larger integrated functional movements. I use parts of this as a diagnostic tool to quickly screen through a patient’s body to help identify dysfunctional movement patterns which helps uncover the driving force of someone’s pain. By restoring imbalances in mobility and stability throughout the body, you increase optimal movement and decrease the strain through the body to allow for tissue healing.
The SFMA is a movement-based diagnostic assessment tool, designed to clinically assess 7 basic movement patterns in anyone with known musculoskeletal pain. The SFMA provides a quick and easy method to systematically find the cause of symptoms by logically breaking down ineffective movement patterns and diagnosing their root cause as either a movement problem or a stability/motor control problem. I use SFMA as both an initial diagnostic tool but also as means to measure your improvement once you have completed your treatment plan.

I believe it is important to be an active member within my professional associations and I take pride in being a vital partner in the say of which direction my profession grows. As a member of the Orthopaedic Division of the Canadian Physiotherapy Association (CPA) as well as the Physiotherapy Association of BC (PABC), I am provided with updated courses and opportunities to continue to improve my skill set and abilities as a physiotherapist. The Orthopaedic Division of the CPA is the leading authority for post graduate orthopaedic training in Canada. Their curriculum is continuously evolving based on an evidence informed model geared towards improving treatment and assessment skills as well as collaborating and learning from a community of expert professionals.
I am also a member in good standing with the Australian Physiotherapy Association (APA) which allows me first access to much of the physiotherapy research which makes Australia one of the foremost leaders in Orthopaedic Physiotherapy.
These associations lead the world in Physiotherapy and continue to advocate and inspire excellence and innovation in our field. I am honoured to be a member of such associations which advocates continued professional growth and development through continued access to information on best practices / education, resource availability and professional networking.

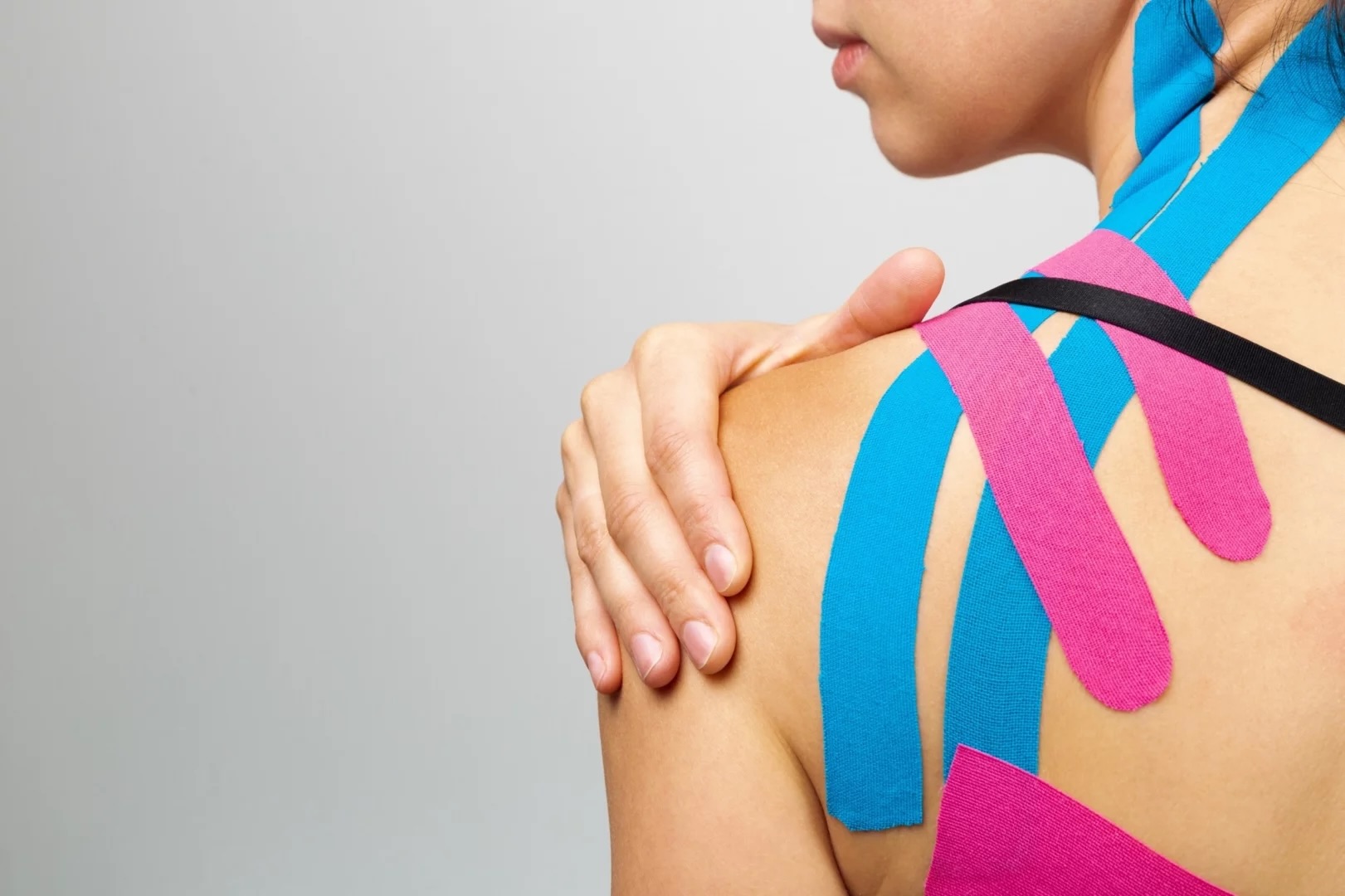
Rocktape, a form of kinesiology taping, involves the application of a specialized, often colourful, hypoallergenic elastic tape designed to mimic the elasticity of human skin. Unlike rigid athletic tape, it allows for a full range of motion while still providing subtle support and proprioceptive feedback. This enables the tape to influence muscle activity, assist with joint alignment, and reduce strain on injured tissues without restricting movement—making it useful in both acute injury management and longer-term rehabilitation.
One of the primary proposed mechanisms of kinesiology taping is its ability to gently lift the skin. This decompressive effect may help improve local blood flow and lymphatic drainage, assisting in the reduction of swelling, inflammation, and pressure on pain-sensitive structures. By enhancing circulation and facilitating the removal of metabolic waste, taping can contribute to a more optimal healing environment, particularly in the early stages of injury.
Beyond its effects on circulation, Rocktape also provides continuous sensory input to the nervous system. This input can enhance proprioception, or body awareness, helping individuals move more efficiently and with greater control. As a result, the tape can be used to facilitate underactive muscles, inhibit overactive ones, and support improved movement patterns. This neuromuscular re-education is especially valuable in addressing chronic conditions, correcting biomechanical dysfunctions, and reducing the risk of re-injury.
Rocktape is not intended to be a standalone treatment, but rather a complementary tool used alongside other physiotherapy interventions such as manual therapy, exercise prescription, and patient education. Its applications are broad, ranging from sports injuries—commonly seen in high-level athletes, including those competing at the Olympic level—to postural dysfunctions, neuropathic conditions, and lymphatic concerns. As with any intervention, appropriate assessment and clinical reasoning are essential to determine when and how taping should be applied to achieve optimal outcomes.